If you suffer from a sleep disorder, you aren’t alone. 50 to 70 million people in the US suffer from a single or more than one sleep disorders throughout their lifetime. Sleep disorders include insomnia, narcolepsy, and, of course, sleep apnea.
Sleep apnea accounts for nearly half of the reported sleep disorders in America. The majority of people diagnosed with this disorder are men. Still, most men don’t know about the connection between sleep apnea and erectile dysfunction.
Erectile dysfunction can be devastating to your confidence and your relationship. Meanwhile, sleep apnea can cause a lack of sleep. This can make your sexual dysfunction symptoms worse while also conferring a whole host of negative symptoms you don’t want to do deal with.
Luckily, there is a solution for men suffering from comorbid sleep apnea and sexual dysfunction. We’re here to tell you all about it today. Keep reading for everything you need to know about sleep apnea, erectile dysfunction, and how testosterone therapy can help.
What is Sleep Apnea?
Sleep apnea is a disorder that negatively affects nighttime breathing patterns. This lack of oxygen alerts the brain, causing abrupt wakefulness throughout the night and leading to poor or too little sleep. Worse, disruptions in your natural circadian rhythm can lead to further health complications.
This disorder comes in three different types:
- Obstructive Sleep Apnea – This is the most common type of sleep apnea, affecting more than 17 million people worldwide. In this type of sleep apnea, the muscles in the back of the throat can’t keep airways open during sleep. Ultimately, this causes interruptions in normal breathing patterns.
- Central Sleep Apnea – In this type of sleep apnea, it’s the brain that fails to regulate breathing, not the throat muscles. The brain fails to signal proper breathing control, and, when breathing lapses, the person wakes up. Over time, central sleep apnea leads to a lower total level of nighttime oxygen.
- Complex Sleep Apnea – A person is diagnosed with complex sleep apnea when they show signs of having both obstructive and central sleep apnea. That means they may suffer from both throat muscle problems and the brain’s failure to regulate nighttime breathing. This is the rarest form of sleep apnea.
As you can see, the two biggest issues with sleep apnea conditions as a whole are sleep deprivation and lack of oxygen.
Combined, these two factors have been shown to up the risk for hypertension and cardiovascular disease. They’ve also been known to affect mood and lead to memory disturbances.
Sleep Apnea Etiology
The cause or causes of sleep apnea aren’t fully understood. Researchers do know that this condition runs in families, though. This implies a genetic component that may influence the development of sleep apnea.
Indeed, individuals with particular physical features are more prone to sleep apnea, too. For example, a small upper respiratory tract, a smaller than average jaw or a large overbite, a large neck size, and a recessed chin shape may increase the risk for sleep apnea.
Other risk factors include obesity, tobacco or alcohol use, age, and even ethnicity.
Symptoms of Sleep Apnea
Chronic snoring is the most common and most obvious symptom of obstructive sleep apnea.
Some sleep apnea symptoms are less obvious, like:
- Waking up with a dry mouth
- Waking up with headaches in the morning
- Difficulty falling asleep
- Difficulty staying asleep
- Hypersomnia (excessive sleepiness during the daytime)
- Difficulty concentrating
- Irritability
All three disorders, though, share in common the periods of completely stopped breathing, followed by abruptly waking up. Upon awakening, central sleep apnea sufferers report feeling short of breath.
Individuals with sleep apnea are also more likely to suffer from depression, problems with learning and memory, and sexual dysfunction (i.e., erectile dysfunction). Some studies report an increased rate of falling asleep at the wheel and automobile crashes in people with this disorder.
How Sleep Apnea is Diagnosed
The gold-standard sleep apnea diagnosis tool is the sleep study. During a sleep study, patients spend the night (or a few nights) in a designated sleep lab. There, they’re monitored throughout the night for blood oxygen levels, breathing rate, brain activity, and leg movements.
Additionally, practitioners use the apnea-hypopnea index for diagnosis. Physicians or researchers use this scale to measure how many times per hour an individual’s breathing pattern is fully or partially interrupted during sleep.
Many patients don’t prefer the laboratory setting. Instead, an at-home sleep apnea diagnostic tool may be used to diagnose this disorder. The at-home test is called limited channel testing, and it can diagnose some patients with sleep apnea all from the comfort of their own bed.
Sleep Apnea Treatments
Physicians typically prescribe CPAP or EPAP devices for individuals with obstructive sleep apnea.
Continuous positive airway pressure (CPAP) and expiratory positive airway pressure (EPAP) devices are worn during sleep. They feature a mask that fits over the mouth and nose to help keep airways open at night.
Other non-invasive methods include using an oxygen tank or wearing an oral contraption that keeps airways open at night.
Of course, there are more invasive methods of treating sleep apnea. For example, tissue removal surgery is a common treatment for obstructive sleep apnea. During tissue removal, pieces of the throat muscle are removed to open up the airways and reduce nighttime breathing disruptions.
There are other types of surgeries your physician may prescribe. However, which ones he or she prescribes depends on the exact underlying cause of your sleep apnea symptoms. Ask your physician if implants, jaw restructuring, or a tonsillectomy could alleviate your symptoms.
Outcomes for Sleep Apnea Patients
With the nightly use of a CPAP device or one of these other treatment regimens, people with sleep apnea can see extremely effective results. However, if symptoms persist, there are a few lifestyle changes recommended for individuals with this disorder. They include:
- Losing weight
- Abstaining from alcohol
- Quitting smoking
Without seeking treatment or making these lifestyle changes, sleep apnea can complicate other areas of life.
However, your physician will also want to address issues that could be exacerbating your symptoms. For that reason, you need to know about the link between sleep apnea and erectile dysfunction.
How are Sleep Apnea and Erectile Dysfunction Connected?
Erectile dysfunction (ED) affects 20% of adult men between the ages of 30 and 70. In this disorder, men experience a reoccurring and persistent inability to have or maintain an erection. The risk of developing erectile dysfunction increases with age.
In addition to age, researchers have found a whole string of other potential causes of ED. These include:
- Certain Diseases – Diabetes, cardiovascular disorders, kidney disease, and multiple sclerosis are all associated with the development of ED.
- Medication – ED is a side effect of many medications, including those that treat hypertension, depression, insomnia, and ulcers.
- Psychological or Emotional Problems – Anxiety, depression, guilt, low self-esteem, fear of failure, and stress have been found to confer a higher risk for ED.
- Other Lifestyle Factors – Like sleep apnea, smoking, drinking, using illicit drugs, obesity, and a sedentary lifestyle contribute to ED symptoms.
Perhaps surprisingly, 63% of men who are diagnosed with obstructive sleep apnea also have erectile dysfunction. Considering that only 47% of men without sleep apnea suffer from ED, this a substantial clue that there’s a bigger connection between these two disorders.
Researchers are still trying to understand the exact relationship between sleep apnea and ED. Yet, what we do know suggests the lack of sleep that is a hallmark of sleep apnea may influence the production of hormones. For example, testosterone.
Sleep Apnea and Low Testosterone
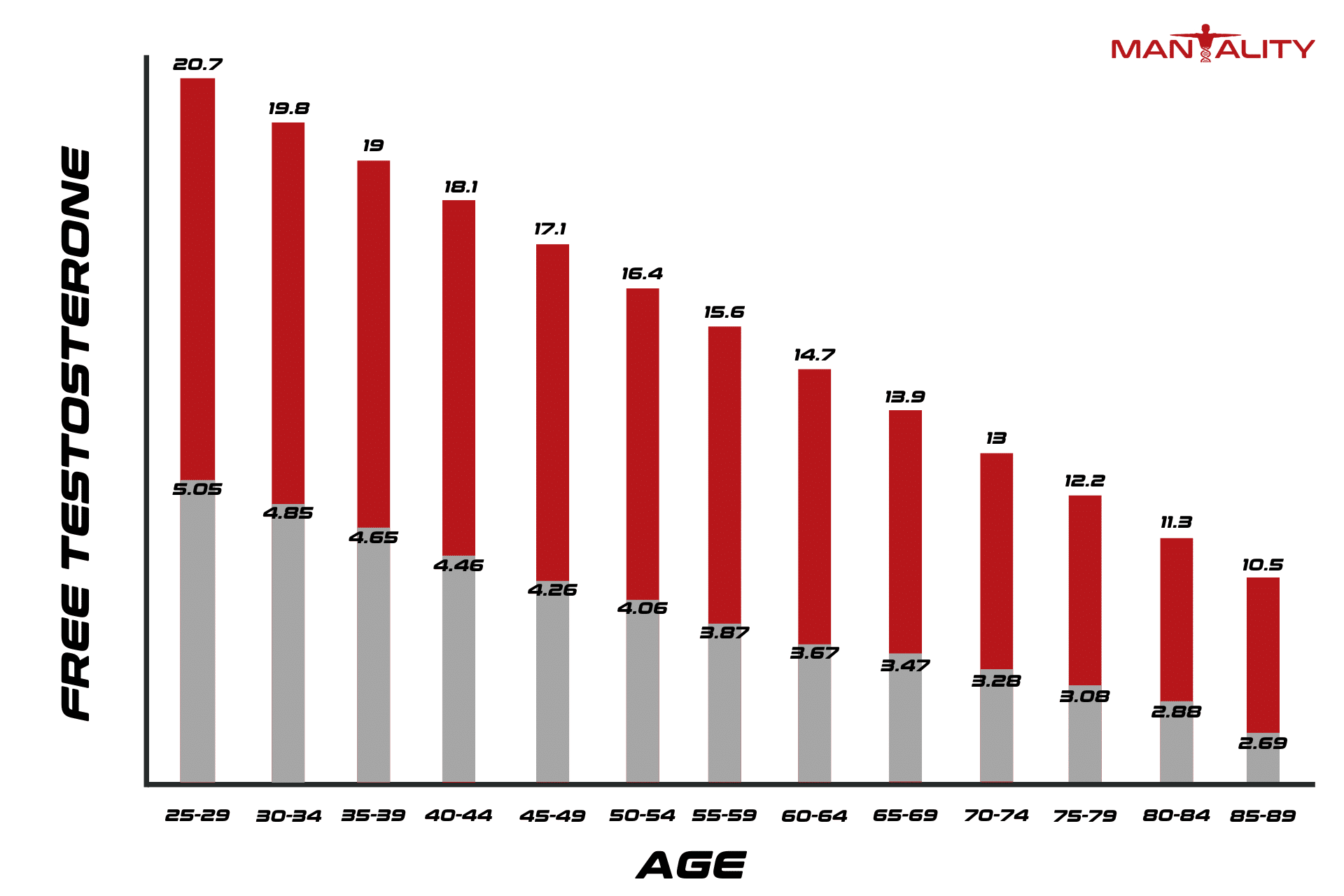
Testosterone is a hormone produced in the brain and released to the body to perform a variety of functions. Throughout a 24-hour day, testosterone production fluctuates. At night, testosterone levels tend to spike during REM sleep, only to begin their decline during daylight hours.
However, when sleep apnea enters the picture, REM sleep is often disrupted. Since the most testosterone is produced during this time, a lack of REM sleep may contribute to lower total testosterone levels. Low T is one of the most common reasons for ED.
There are other signs you may be dealing with low testosterone. Here are some low T symptoms to watch out for:
- Inability to focus or concentrate
- Loss of muscle mass and strength
- Severe depression
- Lack of energy
- Poor libido
- Inability to sleep (which may or may not be associated with a comorbid sleep disorder)
- Weight gain and difficulty shedding fat
There are two factors that are absolutely vital to a healthy erection: testosterone and oxygen levels.
We’ve already discussed the connection between low T, sleep apnea, and ED. Now, let’s explore the reason why oxygen is so important to getting and maintaining an erection.
Erections and Oxygen
One of the scariest parts about having sleep apnea is the period during which breathing doesn’t occur. This restricts the amount of oxygen in the body. Over time, recurring periods of restricted breathing can add up, leading to a chronic reduction in oxygen levels at night.
Studies show that chronic reductions in nighttime oxygen levels can lead to higher rates of ED. In fact, one study looked at this relationship. The researchers found that men with ED have significantly lower penile oxygen levels during an erection than men without ED.
Other Potential Connections Between Sleep Apnea and ED
Another potential reason for the link between sleep apnea and ED? Some experts chalk it up to the stress and fatigue factor.
Sleep apnea often leads to sleep deprivation. As the hours of lost sleep pile up, so does stress and tiredness throughout the day.
No, stress and fatigue may not cause ED on their own. Still, both of these factors may aggravate ED symptoms, making symptoms even worse.
Can Testosterone Therapy Help?
So, what’s the good news? Treating sleep apnea has also been shown to reduce the symptoms of ED in men. One study even showed the benefits of CPAP devices for improving erections.
However, these results need to be validated with more research.
In the meantime, there may be a better option for men suffering from low testosterone due to sleep apnea.
Testosterone replacement therapy (TRT) is a tried and true way to treat the negative symptoms of low T, including erectile dysfunction. Here’s how it works.
Testosterone Replacement Therapy Methods
The point of testosterone replacement therapy is to increase levels of low T. A medical professional does this by prescribing a testosterone replacement medication. These medications come in tablets, pellets, topical creams, and intramuscular injectables.
We recommend testosterone injections because they allow for more precise dosing and administration to a more specific location. A medical professional administers the injection into muscle tissue, which makes the process relatively painless for most men.
The time it takes for the therapy to work differs among men. Yet, most TRT patients see results within 3 to 16 weeks after the initial dose.
Testosterone Replacement Therapy for Men with ED and Sleep Apnea
Sleep apnea and erectile dysfunction combined can be absolutely devastating to your health. Know that you’re not alone and these diagnoses can be treated with the help of your physician.
The first step toward recovery is making an appointment with your physician to talk about your symptoms. After that, you can get the treatment you need for relief.
That’s where Mantality Health comes in to help you!
Are you looking for testosterone replacement therapy to help with your ED and sleep apnea diagnosis? Find a Mantality location near you and fill out our convenient contact form to set up your appointment today!